|
Early pregnancy can be a time filled with many different emotions. I was so shocked and grateful to be pregnant that I didn't want to admit that pregnancy is tough. Your body is growing a literal human and that takes an enormous amount of energy. Make sure to give yourself grace in the process and the freedom to experience it in a balanced, rounded way. Pregnancy hormones (HCG, estrogen, progesterone to name a few) can produce a variety of symptoms. Each person experiences first trimester differently but here are some of the most common ones: Morning sickness (all day sickness for many), food cravings/aversions, frequent urination, insomnia, bloating, headaches, anxiety, feeling hot/heart beating faster, mood swings and fatigue. I decided to write this post as an encouragement to those in their first trimester. In my experience (I was 9 weeks pregnant as I started to compile these tips!) first trimester can be a time of great excitement, shock, joy, overwhelm and even loneliness. Many people choose to wait until the end of first trimester to tell family and friends and it can leave people feeling alone in their fatigue/nausea etc without experienced-mother-friends to lean onto for support. Many women don't see their midwife or OB until the 8-week mark or even later and that leaves many weeks of navigating the changes to your body on your own. These are some tips I've learned along the way and hope it is helpful to anyone going through first trimester keeping it a secret <3 You are seen, you are loved, you are capable, you are growing a human and that takes a lot of energy, emotion and sacrifice. You are incredible and your body was designed to create, grow, nourish and birth this baby <3 You are never alone. Tips for common pregnancy symptoms as outlined above that has worked (or at least helped A LOT) for me. Some may seem silly but if you're in the throws of first trimester like me, you might feel like trying anything to help you through. Also note that it is always wise to keep in communication with your midwife or OB and this is not prescriptive advice just encouragement and tips from what has been helping me. If you are dealing with more severe symptoms of any kind (mental or physical) always reach out to your provider for additional tips. Good luck!
Lastly, Know that first trimester symptoms largely go away by second trimester but that may not be at 12 weeks (like all the apps and friends say!!).. or 13.. or 14. For me I have felt much better since around 14.5 weeks and I am finally enjoying some long-awaited 2nd trimester bliss! You can do it! You are doing it. You are stronger than you think. You are the best mama for your baby. Blessings, Michaela Helpful encouraging video: (3) HOW TO SURVIVE THE FIRST TRIMESTER: My 10 Step Routine! - YouTube
0 Comments
“Doulas empower you to make informed choices during pregnancy & birth and encourage you to trust in your body's ability to birth”
I have paused my doula business for now to pursue other roles (check out my About Me section to learn more!) so I have decided to share my template I created to help mothers and families start to envision their birth. I hope you find this to be a good launching pad for preparing for your birth! Let’s get started! Envisioning your baby’s birth…
This is a template to introduce different types of interventions & comfort measures. Some are specific to hospital settings. Feel free to ask me any questions to clarify options/help you make an informed decision when planning!
Consider including a line that says something similar to: THANK YOU to my nurses and doctors/midwives for taking such good care of me! I also encourage you to write (potentially on a different sheet of paper if birthing in a hospital) how you envision the space in terms of lighting (dim/bright), comfort measures you’d think you’d like/dislike, how you envision your partner/doula helping you, labor project? Postpartum planning? Etc. Use the birth support sheet as a guide! Remember, this is your body, birth, & baby. You always have a choice for interventions, place of birth, midwife or OB, and you can always change your mind. Creating a Birth Vision instead of a Birth Plan may allow you to be open minded to the unpredictability of birth. You can write this the way YOU WANT to. You can go into as much or little detail as you’d like. Sometimes, it is helpful to keep it less than one page double spaced and include only what you’d really like the doctors, nurses, midwives to know about you and your wishes. Medical providers, especially in the hospital, generally have more than one pregnant woman in labor so the more concise the more likely they are to read it, remember it and respect your desires. Happy birthing! Michaela Many women find that bringing their babies into the world in a calm, home-like atmosphere has powerful benefits for both them and their babies. Birth can be one of the most transformative moments of your life. It is crucial to birth in a setting that you feel the safest to allow your body to relax, release tension, and surrender to the process. Depending on the city in which you live, there may be a birthing center staffed by Certified Nurse Midwives. You are encouraged to move freely, use the bathtub or shower for comfort and progress of labor, eat and drink as you wish to keep your energy up and stay hydrated. You are able to have whoever you’d like at your birth, labor in a comfortable, quiet environment with minimal interruptions. It is such an intimate experience to bring your baby into the world and feeling comfortable with privacy is important for reducing fear and increasing relaxation. The Shift from Home to Hospital In the early twentieth century in the United States, the majority of births shifted from home to hospital (nearly all births were at home with a midwife in 1900, 50% by 1938 and less than 1% by 1955). One of the motivations for doing so was to take away pain in childbirth by introducing general anesthesia and to decrease infant and maternal mortality rates by having a more sterile environment. However the decreased mortality rate for both mom and baby has largely been attributed to the medical advancements to helping high risk women birth safely and the availability of antibiotics when needed during pregnancy, labor or early in the infant's life. The use of general anesthesia is very rare now and women since the 1970s have been trying to regain control in their birthing process. Although most births in the US occur in the hospital, there is a shift happening again back to more home and birthing center births (increasing since 2004, and increasing massively in 40 states since 2020). The safety of homebirth has been studied and is not widely known. The factors that make home birth as safe as hospital births in numerous studies include home births with; a trained midwife attending, adequate prenatal care, healthy mom and baby, and having a hospital close by. Some studies showing that home births are less safe include free births with no medical provider, births that happen ‘outside the hospital’ by accident. ie. In the car on the way, high risk births etc. Home births and birthing center births are more common in other developed countries and are shown to be a safe option with less medical interventions for low risk women. Benefits of Planned Home or Birth Center birth:
For an inside look into birthing suites and to learn more about the birthing center experience check out some of my favorite pages!: Welcome to Birth Center of Chicago (Chicago) Birth Option (midwifecenter.org) (Pittsburgh) Hygge Birth and Baby | Denver Birth Center (Denver) Transferring to the Hospital Most planned home and birth center births transition to the hospital setting in a non-emergent way due to the mother requesting pain medication and labor dystocia (long labor). According to a systematic review of the literature in 2014, "Fifteen studies were eligible for inclusion, containing data from 215,257 women. The total proportion of transfer from home to hospital varied from 9.9% to 31.9% across the studies. The most common indication for transfer was labor dystocia, occurring in 5.1% to 9.8% of all women planning for home births. Transfer for indication for fetal distress varied from 1.0% to 3.6%, postpartum hemorrhage from 0% to 0.2% and respiratory problems in the infant from 0.3% to 1.4%. The proportion of emergency transfers varied from 0% to 5.4%." (1) What do health organizations say about this? The AAOG's (American Academy of Obstetrics and Gynecology) current stance is that a hospital or birth center is the safest option but that women should be educated on the risks and benefits of all birth options and should be able to make a medically informed personal decision on place of birth. This stance changed in 2014 from stating that birth should always be done in the hospital setting to recognizing home and birth center births as a valid choice for place of birth. (2) The ACNM (American College of Nurse Midwives) states that women should be educated on all birth place options and have the right to access safe home-birth options. Its position is based on numerous studies from other developed countries who have a highly integrated maternity care system to include planned home births (3). Home and Birth Center birth is shown to be just as safe as hospital birth for low risk mothers- but with less medical interventions, continuous fetal monitors that limit movement, interruptions, machines beeping, and paperwork! The worldwide statistics from the WHO regarding out of hospital births show it is safer to give birth in a hospital setting where access to a clean, safe environment for women with inadequate prenatal care, nutrition and education is beneficial. Home and birth center births are shown to be equally as safe with less interventions when there is a medical professional present, in a clean home or center with birth and emergency medicines and supplies available and when a timely transfer to the hospital is possible. This is not possible in areas that lack transportation and resources to provide this type of care. The WHO is working to increase access to maternal health care worldwide and currently the hospital in many countries is the safest option. However, in the US and many European countries where midwifery care is more integrated, home births have been shown to be a good option for low risk pregnant women. Birth doesn’t need to be seen as a high risk medical event, but a natural process that can be monitored and only intervened in when necessary. “Only rarely do doctors in training have the opportunity to sit continuously with laboring women for hours. Most are taught to intervene in the normal process so often and so early that they have never witnessed a normal labor and birth.” - Ina May Gaskin, midwife and author of Ina May’s Guide to Childbirth. Many people are not aware that they have a choice in where to birth their baby. I am an advocate for out of hospital births for low risk women because I have seen the benefit of birthing in a comfortable, dimly lit, peaceful environment where interruptions are minimal. That setting allows the mother to relax and trust her body's ability to birth. I hope this has been helpful to those searching for another way to approach women’s health care and birth- one that is personal, intimate and empowering! References & Resources: (1) Transfer to hospital in planned home births: a systematic review | BMC Pregnancy and Childbirth | Full Text (biomedcentral.com) (2) Planned Home Birth | ACOG (3) ACNM Statement on Practice Settings – 2005 (midwife.org) National Birth Center Study II - American Association of Birth Centers Outcomes of planned home birth with registered midwife versus planned hospital birth with midwife or physician - PMC (nih.gov) Home Births Gain Popularity in ‘Baby Bust’ Decade | Healthiest Communities Health News | US News What is Home Birth? - Evidence Based Birth® September's Blog Post features a guest writer! Jan Mallak was my doula trainer and has a passion for teaching others about the health benefits of breast milk and the donation process for mothers and babies in need. This post is geared towards doula's learning about the importance of education their clients on milk donation, however all people can learn about the process and share the knowledge to help more babies by spreading the word!
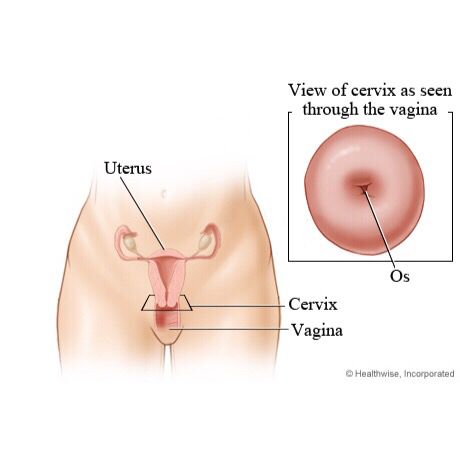
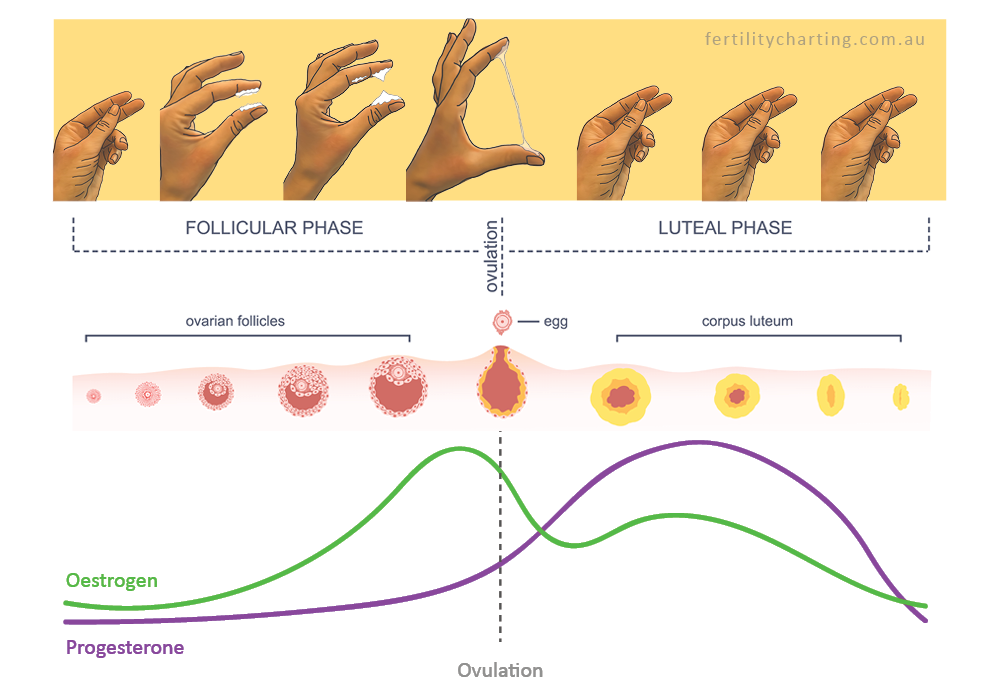
This month we are celebrating the mothers who have devoted time and energy to donate their extra breastmilk to a milk bank! Milk banks provide donated breast milk to babies in need. It is truly a gift so thank you! If you are a mother who breastfeeds and has extra supply in your fridge or freezer, consider donating to your local milk bank Human Milk Banking By: Jan Mallak As doulas, we are expected to offer physical, emotional, spiritual, mediatorial and informational support. Part of informational support is providing childbearing related resources to your clients. Doulas can become “connectors” in the birthing community because of the many relationships they develop with complimentary maternity care providers. So, Resource Lists are often complied by doulas to give to clients, colleagues, and staff. Educating those we encounter is a great way to make them aware of the many options available to families. Perinatal listings of local resources can benefit the mother before, during and after her birth experience. So, the list should include everything from prenatal exercise to breastfeeding assistance (and many in between). One of the several resources you should include is Human Milk Bank information. Western Pennsylvania is very fortunate to have the Mid-Atlantic Mothers’ Milk Bank (located at 3127 Penn Ave. Pittsburgh, PA 15201 phone 412/281-4400). I say fortunate because there are only 31 accredited human milk banks recognized by HMBANA in Canada and the United States. The Three Rivers Mothers’ Milk Bank opened in 2016 after 2 years of finding a location, doing necessary construction, securing a Board of Directors, hiring/training staff, purchasing the required items for collection/storage/processing/shipping/etc., connecting with all the health care providers/centers, raising substantial funds to support the project and meeting international (HMBANA), state (PA) and city (Pittsburgh) legal/organizational requirements. The name was later changed to the Mid-Atlantic Mothers’ Milk Bank because of the expanded regions of service. I had the honor of being involved with the MAMMB from the very beginning. One of my doula clients (Denise O’Connor) decided to initiate the vision of having a milk bank in Pittsburgh. She approached me to be on the founding Board of Directors and I accepted. After all, how could I refuse when she asked me if I wanted to help save babies lives? So, I became the first Executive Board Treasurer. Of course, being on the Board included many other volunteer duties. During my 6 years of serving, I also coordinated the first conference hosted by the Milk Bank, developed/implemented/facilitated Lost & Found (perinatal loss support group formed to help bereaved donors) and wrote a children’s book called An Ounce of Sharing … at the Milk Bank. The book is about Lizzie who just became a big sister. It takes the reader on a tour of a typical milk bank through her eyes. It explains processing and distribution of milk from donor to recipient. And Lizzie also learns that helping others, especially fragile babies, makes her feel happy. It is given to all donors as a thank you gift and serves as an educational tool for schools/libraries/hospitals/doctors’ offices/etc. The book’s “for parents and professionals” section has recently been updated so other milk banks can purchase it from the MAMMB. It can also be bought on the Mascot Book website (mascotbooks.com) and Amazon. All the profits made by the sale of the book are my personal gift back to the Milk Bank. If there is a milk bank near you, try and go for a tour. The staff can show you the frozen milk that is received, defrosted, processed, and refrozen for distribution. Seeing the laboratory conditions, the testing utilized to ensure a safe product and the organized manner of delivery to hospitals or individual patients is quite impressive and educational. Donor milk is distributed by prescription or hospital order only. Donated milk can be dropped off at the milk bank/depots or shipped free of charge. The processed milk is available for pick up or overnight delivery. In general, these are the steps for donation and milk processing: 1. Donors must be healthy mothers who make milk beyond their needs. They must go through a screening process that includes a phone interview by staff, completion of a medical history form, a statement of health from both the mother’s and baby’s doctors and blood testing. 2. Once the donor is approved, her milk arrives at the milk bank frozen in bags or bottles. 3. Before processing, the milk is thawed in a refrigerator. 4. The thawed milk (sometimes from several donors) is mixed and bottled. 5. The bottles are placed in a warm bath pasteurization unit. All HMBANA milk banks use the Holder Method of 145 degrees Fahrenheit for 30 minutes. This eliminates pathogens while maintaining as much of the bioactivity as possible. 6. After completion, bottles are cooled and labeled. 7. A random bottle from each batch is cultured for bacteria. 8. Milk analysis and drug testing can also be done if the milk bank has those capabilities. 9. Processed milk is stored and shipped frozen. 10. Expired milk cannot be used for recipients. The expiration date on donated milk is one year after pumping if stored in a freestanding freezer. Less if stored in a freezer/refrigerator combination. But expired milk can be used for research. In fact, the Mid-Atlantic Mothers’ Milk Bank has a BioLab on site for just that reason. Most donor milk is used by infants in the NICU at hospitals. In the U.S., one in nine infants are born prematurely. Up to 12% of significantly premature babies can develop an inflammation of the intestines called NEC (necrotizing enterocolitis) and half of these babies require surgery. The use of human milk can dramatically reduce these numbers … incidence of NEC by 80% and need for surgery by 90%. Nearly 70% of mothers of preterm infants cannot provide enough milk for their baby’s initial needs. So, the “bridge milk” provided by milk banks can be used until the mothers can establish a good milk supply. Then, the baby can transition from the bottle to her breasts by discharge. What can you do as a doula to support milk banking? Be able to describe basic milk banking procedures. Provide educational materials to your clients about milk banks. Inform other birth professionals about milk banks. Encourage and support your client’s decision to donate. If needed, connect your client with a milk bank for an inpatient or outpatient reason. Be mindful of maternity/lactation related legislation that may be pending in your state. And celebrate World Breastmilk Donation Day on May 19th in a special manner. You will be helping to save babies’ lives in these ways. And that is one of the most rewarding aspects of being a doula! As you prepare for your birth, it is just as important to envision how you will spend the first days and weeks postpartum. This is an exciting but demanding time and when planned for thoughtfully, you invite the possibility of feeling more rested, balanced and able to care well for your new little one. It is also a time of huge transition for fathers/partners and allowing for time to bond as a family gives everyone an opportunity to transition well. Your focus is on healing physically, bonding, nursing and resting. Partners often worry about how they can help, how they can bond with baby and what to do in the early postpartum days. Being present is the key. Being there to listen, support and comfort is essential. Partners can do this by preparing nourishing foods- or ideally heating up what lovely friends/family have prepared!, bringing hydrating drinks, and simply being an encouraging presence. Dads who do skin to skin reap so many benefits of bonding that mother’s experience! -that is another whole blog post though. I believe it is a beautiful, sacred time that has the power to transform your family just as much as the birth of your child does. Let’s dive in! This period is often called the fourth trimester because it is a time that requires deep rest and healing; physically, mentally and emotionally. Your body just created, grew and birthed your baby and placenta and it is important to honor your body and baby by giving yourself and your little one the best opportunity to flourish. Postpartum depression is highest in countries (including the US) who don’t encourage and support women in their time postpartum by allowing for rest. These high depression rates affect bonding, feeding, and overall ability to mother well and transition as a couple into parents. In chinese culture the first forty days postpartum is called the ‘sitting in’ period where the new mother is cared for with nourishing foods, oil massages, and warm teas. Her focus is to rest, heal, nurse and bond with her baby. This has been modified in recent years to gleam the essence of the rest period and value the importance of it while giving it a structure more conducive to families today. What is highly recommended by midwives today is called honoring the “5-5-5 Rule.” This is when women spend 15 days focusing on resting and getting to bond with and feed their newborns. Some people call this planning for their “baby moon.” Remember: It is not selfish to rest, you just birthed your baby and placenta and your uterus needs time to close and heal well. This is actually the kindest thing you can do for your baby! These are some examples of what this looks like and can be changed to suit your family best. 5 days in the bed: This is where you spend your first 5 days lying in bed focusing on resting, sleeping, skin to skin and nursing your baby. Ideally your partner (or another type of supportive person: mother, mother in law, doula etc) would bring you nourishing foods and plenty of water and teas to stay hydrated. You can read, watch TV and invite a few visitors if you’d like but keep the activities to a minimum. Don’t worry about getting up to shower (unless you feel up to it), your baby actually loves your natural smells and feels safe and warm in your arms. 5 days on the bed: This is time spent on the bed. You might start to sit up more, stretch a little bit, and do activities on the bed (puzzles, card games, etc). You can choose to move to the couch or chair but mostly resting. 5 days near the bed: Continue to take lots of time to sleep and have cuddle time skin to skin with your baby. This time is focused on resting as much as you feel like and being near bed to take naps frequently. You can start to go for short walks around the block but limit time standing to less than 30 minutes and listen to your body. You won’t be able to care well for your new baby if you aren’t healing physically and emotionally. This is a beautiful time and even two weeks of rest makes an enormous difference in your transition into motherhood and giving yourself and family the best opportunity to flourish. Resources: There are wonderful postpartum planning tools such as which I highly recommend to get you started in the planning phase! And as always, please read Ina May’s Guide to Childbirth (2019) if you haven’t already. It will change your life! Postpartum Planning + Support Bundle | Beautiful One (beautifulonemidwiferysandiego.com) How to Make a Postpartum Plan (Plus a Free Template!) - Baby Chick (baby-chick.com) Book I recommend & my review: The First Forty Days: The Essential Art of Nourishing the New Mother (Ou, 2016) A sweet collection of wise advice from Chinese mothers passed along generations and refreshed into modern ways of balancing life as a new mother. The importance of rest, warmth, and nourishment in the first forty days was emphasized with loving stories and recipes. This book can be used as a tool for pregnant women and their support people to welcome the baby and new mother into the world. The tools in this book help to inspire you to think deeply about the sacredness of the first month postpartum and how asking for help and creating space to lay low with your baby is important for initial and life long mental and physical wellness. Overall a very soothing read 💕  Many women (including myself) were taught (minimally at best) about our menstrual cycles and reproductive systems as we hit puberty. We gathered some information from our friends about how long periods usually are and we started to notice how our moods change throughout the month (not to mention the cramps!). This post is not about how to ease PMS and regulate hormones for better cycles (although that topic is coming up in a few months!). This post is about something that was never explained to me nor many friends and doula clients I’ve talked with: cervical mucus! Where is my cervix and what does it do? Your cervix is the end point of your uterus and keeps your womb closed. It looks and feels like a small, squishy, wet, pink, donut. The opening is called the cervical os. It is also the top end of your vaginal canal and where sperm go through (they are very tiny) to create babies (if I went through all of those details this would be too long of a post haha). The cervix is also what softens, thins (effaces), and stretches (dilates) during labor to allow your baby to be born through your vagina. Many women believe in the connection between your throat and your cervix. When you moan or breathe deeply (during sex or while relaxing in childbirth), your cervix then also softens and opens. This article The Wisdom of the Cervix explains this connection (with images) in more detail. Is vaginal discharge normal? Cervical mucus changes throughout your cycle and can indicate when you may expect your period or when you are nearing ovulation. It is a completely normal, healthy and important part of our reproductive lives. It can be dry/scant (before & sometimes just after your period), thin/watery or thick/creamy (between period and ovulation), then it becomes VERY slippery/wet resembling egg whites near and during ovulation (usually 1-3 days), and then dry again until your period. There is a WIDE range of normal and everyone is different. You can notice cervical discharge on your underwear, on a tissue as you wipe after peeing, or you can feel your cervix for mucus. Cervical mucus is usually clear to white depending on its consistency. If you notice discharge that is green, yellow, other funky colors, has a strong odor or just seems different to you it could be a sign of a yeast infection, vaginal infection or STI/STD and it would be recommended to see your OBGYN, Nurse Practitioner, Midwife (whoever you see for your yearly visits. Can I check my cervix to learn more about my body & cycle? If you have never felt your cervix I highly recommend it! Your cervix is usually high up in your vagina during ovulation and remains high when pregnant. After ovulation, if not pregnant, it will move down slowly and just before your period it will be very low in your vagina and easily felt. In the shower (recommended because you have very clean hands and privacy), you can lean over slightly as you would to insert a tampon or menstrual cup, stick your middle finger inside your vagina until you feel your cervix. It is usually doughy and feels like you are touching the tip of your nose. (The feeling of your cervix also changes from softer to more firm throughout your cycle). Cervical Checks During Labor: During labor Doctors/Midwives usually recommend cervical checks to feel for progress of labor. Keep in mind that is tells you how effaced and dilated you are right then but not necessarily how much longer labor will be. You can dilate from 6 to 9 in a matter of minutes or it can take hours. The benefits of cervical checks during labor are to check for progress, if you feel like pushing but are maybe not far along in labor yet it can be important to wait to push if not fully dilated to 10cm. The risks of cervical checks during labor is that is can be discouraging to be working really hard and be told “you are only 3cm dilated.” That mental discouragement can really derail your mental focus, concentration and stamina. Each cervical check also increases risk of infection. You can always decline cervical checks or ask your provider what they are checking for and to give you more information on the pros/cons in your situation. Tracking Your Cycle I honestly didn’t know this was a normal, healthy part of our cycles until I studied nursing in college. I hope this post educated you a little more on the role of your cervix and maybe even sparked an interest in you to learn more about tracking your cycles! I have been using the OVIA fertility app to track my periods and cycles for a year and I definitely recommend it. The app includes a lot of encouragement and educational tips throughout your cycle. It is especially useful for TTC (trying-to-concieve) but I’ve found it very empowering as I learn more about how my body was beautifully and wonderfully created (hormones and all!). It teaches you about the different phases of your menstrual cycle, when to expect your period, ovulation signs as well as tips on tracking cervical mucus. Here are some resources if you’d like to learn more! Cervical Mucus: Chart, Stages, Tracking & Fertility (clevelandclinic.org) Cervical Mucus Chart: Know When You're Fertile - Mama Natural Cervical Mucus Gallery (fertilitycharting.com.au) Definition of reproductive system - NCI Dictionary of Cancer Terms - NCI The Connection Between the Cervix and Throat and What You Need to Know About Your Cervical Health (goddessceremony.com) Vaginal Discharge: What's Normal, What's Not (for Teens) - Nemours KidsHealth Many people in the United States are curious about the difference between doulas and midwives. The simple answer is that a midwife is a medical professional who helps women deliver babies (in this definition it is most similar to an obstetrician) and a doula is a non-medical support person who helps women and their partners (emotionally, physically, mentally, spiritually and informationally) prepare for birth and postpartum during pregnancy and helps them know and understand their choices. Doulas are there to educate you on all your choices and support you no matter what you choose. It is your body, birth and baby and we are there to support you to have an empowered birth experience. To learn more about doulas feel free to read my welcome & doula research page on my website! If you are desiring a low stress, peaceful, safe, empowered pregnancy and birth experience then a midwife might be a good choice for you. Midwives typically take a holistic approach to pregnancy, birth and postpartum. Midwives have extensive training and experience in normal pregnancy and birth and can care for you throughout your whole journey, from routine yearly women’s health visits through pregnancy, birth and beyond! Midwives are sometimes registered nurses who go for several years of schooling to become Certified Nurse Midwives. Other midwives are highly trained alongside community midwives. Midwives take the time to talk through nutrition, exercise, postpartum planning and so much more. They can help women in birth centers, hospitals and at home. Some midwives choose to work in one of those places and others have a combination of experience in various birth settings. You can choose to see a midwife for women’s health care too! I made the switch to seeing a midwife at the local birthing center instead of a gynecologist and have appreciated the calm, comfortable conversations and the time they take to educate me on my choices. They care about my holistic health, not just physical but also emotional and mental. When I saw a gynecologist, it was in a typical doctor’s office with bright fluorescent lights and a hurried pace of keeping on schedule. I was thrilled when I learned women’s health care can look different. I can receive care in a peaceful, comfortable room with soft lighting and calming colors. I feel more confident in that setting, asking questions, knowing that she can and will take the time to listen. There are birthing centers in many cities throughout the US that do well-woman visits as well as prenatal care. Remember, you can always make a switch in provider and place of birth. In the US most women go to see a gynecologist for yearly visits, pap smears, birth control, education and then when they become pregnant, they get matched with an obstetrician who will be their prenatal and labor doctor. However, in other countries such as Germany, UK, Canada, Australia, Denmark etc midwives not obstetricians are often the primary medical professional for women's health including pregnancy and birth. Women’s health care and prenatal care should always make you feel comfortable, informed, safe and empowered to make confident choices. It should be a partnership and not make you feel rushed and uncomfortable asking questions. If you want a low intervention, peaceful birth, consider having a midwife as your women’s health care provider and continue to have her support you through pregnancy and birth and postpartum. Midwives are holistic and believe that birth is a normal physiologic process and is safer when not intervened in unless needed. If you’re interested in learning more about midwifery care, I encourage all my clients and friends to read Ina May’s Guide to Childbirth. It is a warm, inviting, honest and beautifully written collection of birth stories as well as research-based chapters on tips for decreasing chances of tearing, how to choose a care provider and place of birth, and tips for comfort measures during labor and ways to prepare your body during pregnancy and labor for birthing your baby. I will continue to re-read this book! Blessings, Michaela Resources for learning more about the safety and prevalence of midwifery care! • Chart: U.S. Midwife Workforce Far Behind Globally | Statista Nursing and midwifery (who.int) The U.S. Needs More Midwives for Better Maternity Care - Scientific American Our Philosophy of Care | Our Philosophy of Care (midwife.org)  Many women are nervous about the pushing stage and are curious about ways to decrease tearing. In some cases, despite 'doing all of the things,' tears happen. You are not a failure, you didn't do anything wrong, it can just happen sometimes. However, there are a lot of ways to help decrease that risk and we will explore some of those today! This month we will discuss ways to let go of the fear of tearing and promote healthy ways to prepare mentally and physically for the pushing stage of labor. In Ina May’s Guide to Childbirth there are numerous birth stories and a detailed chapter about pushing that have helped many women increase their awareness of how their bodies were created and how to prepare mentally for birth. How will my baby’s head fit through that tiny space? This is probably the most common question pregnant women wonder about and it is a very reasonable thing to ponder! My hope in writing this post this month is to educate you on how the female body was designed for birth and empower you to know you have some extra tools to prepare yourself mentally and physically for your birth! Some people are quick to share their painful birthing experiences and it can make it harder to prepare yourself for your own labor if fear is getting in the way. I heard recently that labor is like fitting a watermelon through a nostril! Firstly, your baby is a little soft, mushy, malleable sweetness- not a large, hard melon! Secondly, your nostril was not designed to stretch like a muscle. Let’s explore how your body was created for birth:
Tips for Decreasing Risk of Tearing:
Lastly, a bit of doula encouragement for surrendering in transition and promoting peace in the pushing stage: Soften, Open, Release, lower your jaw, unclench your teeth, release your tongue from the roof of your mouth, soften your lips, lower your shoulders, take a deep breath, open your palms, lean into it and let go. You got this! Happy Birthing, Mamas! Peace & Blessings, Michaela I grew up with parents who believed nutritious foods promote healing & wellness. We took medicines occasionally when needed but it was always combined with natural remedies. When I had the flu recently, I was surprised how many friends hadn’t heard of some of these tips & tricks for promoting healing naturally. I hope you find these to be helpful!
There are many ways to promote immune health and help you recover from a cold without taking medications (which aren't recommended during pregnancy). One of my top tricks for stopping a cold in its tracks or helping myself recover more quickly once it has come on is to EAT RAW GARLIC! What are the Benefits of Eating Garlic?
without OTC Medications:
References & Resources: 11 Proven Benefits of Garlic Health Benefits of Garlic for Kids Date palms are large trees that can produce up to 1,000 dates a year. They were the most common type of palm trees in the middle east during the time of Jesus. It is believed that it was the date palm leaves that were waived as Jesus humbly entered Jerusalem prior to his death and resurrection. Date palm trees are referred to throughout the old and New Testament to symbolize life, victory, righteousness, beauty and fertility!
The leaves and branches were used in the Ancient Greek and Roman cultures for making baskets, buildings and the fruits were eaten as a part of their meals. “The first reference to the date palm is when the children of Israel entered the desert after leaving Egypt (Exodus 15:27). Here, at Elim, they encountered palm trees just as a visitor in many parts of the Sahara today would find oases marked by palm trees.” (3) What Makes Dates a Superfood? Dates are considered a superfood because they are packed with vitamins and minerals that help with immune function, heart and brain health, the development of healthy bones, the regulation of hormones and can even help prepare your body for labor! Packed with Vitamins & Minerals! Dates are rich in iron, potassium, selenium & fiber- among many others! Iron rich foods help prevent anemia and increase energy. Especially when pregnant it is important to increase the consumption of iron rich foods. Your blood volume increases by about 45% when pregnant! (2) Other iron rich foods include red meats, liver, eggs, spinach, pumpkin seeds. Potassium in dates help to relax blood vessels, regulating normal blood pressure. Potassium works with sodium in your body to create a good balance of hydration in and around your cells. Try a refreshing glass of water with a pinch of salt and a slice of potassium-rich fresh lemon to boost hydration! Other good sources of potassium: bananas & leafy greens. Selenium is a mineral that acts like a powerful antioxidant in your body that has been shown to boost our bodies immune response making it easier to fight diseases. Other good sources of selenium are tuna, sunflower seeds, eggs, chicken, and sardines. Fiber helps to prevent and solve constipation issues- so common as a result of a typical American diet (high in sugar, low in fiber) and also in pregnancy! How can dates help prepare my body for labor? Eating about six days per day in the last four weeks of pregnancy has been shown to decrease labor time and help to soften the cervix. The softening of the cervix decreases the need for Pitocin (the artificial form of our naturally occurring oxytocin) to induce or augment labor. (1) Check out my blog post Pitocin vs Oxytocin to learn more! How can I eat more dates for all these health benefits?!
References & Resources:
 What is water birth? Water birth is when you get into a bath of warm water anytime during the first stage of labor and stay in the water during the pushing stage, or second stage. The baby is then born under the water and brought to the surface. The woman can stay in the water for the third stage of labor (birthing the placenta, usually about 15-30 min after birth) or come out of the water and into the bed. A land birth is when you give birth on dry land. You can use water as a relaxation tool whether you deliver your baby in the tub or not. Many of the benefits of water birth can also be seen when using hydrotherapy during labor. What is hydrotherapy? Hydrotherapy is when you are immersed in water during labor. According to the most recent Listening to Mother’s survey, a national survey of women’s experiences during labor and birth, most mothers described the pain relief of hydrotherapy as being more effective than opioids! This decreased use of pain medication leads to less medical intervention and risk of fetal distress. Ways to use water during labor for its powerful benefits:
What are the benefits of water birth?
Won't my baby swallow water during birth? When babies are born they are still receiving oxygen from the umbilical cord attached to the placenta until they are brought to the surface and come into contact with air. They will then begin to use their lungs to breathe. Is water birth safe? Although there are still many providers who believe water birth is unsafe, the evidence of numerous large scale studies show there has been no difference between land and water births when researched about the risk of low apgar scores, respiratory distress or infection. Women who are in preterm labor, have an infection, or if severe meconium is present in the pool, should consider changing to a land birth. Always feel free to have a conversation with your midwife/doctor about the benefit and risk of waterbirth for your unique situation. If you’re desiring to have a normal, physiologic water birth or would like to use water as a comfort technique, know that the evidence overwhelmingly supports the use of water during labor and if you’re doctor says as a rule “it’s unsafe and not allowed,” you can always find a new doctor or switch to a midwife who knows the benefits and will support you! It is important to make sure the birth tub you use is cleaned before use. Can I have a water birth in the hospital or only if I have a home birth? Water birth and hydrotherapy can be used in any birth setting with running water: hospital, birth center, home. Many hospitals are becoming more ‘baby/mama’ friendly but be sure to be clear from the beginning that you desire the ability to have intermittent monitoring or doppler use so you can be free to take a shower or bath. You can have a normal, physiologic birth using water or water birth as one of your tools for achieving a relaxed state wherever you give birth. When choosing a place to give birth and a midwife or doctor, make sure to ask specific questions about availability of showers/tubs and whether the provider supports you in the use of it. Common Questions:
When is best to shower or take a bath in labor? The actual answer is: Whenever it feels natural to you! But these are some helpful things to keep in mind from experience and research!
If water birth intrigues you, have a conversation early on with your midwife/doctor about how to plan for that. You can always decide to have a land birth if that feels right during labor. As you are giving birth to life, don’t forget about the basic element that sustains life on earth: water! References & Resources: Birth, Bath, and Beyond: The Science and Safety of Water Immersion During Labor and Birth - PMC (nih.gov) Water Births | the American Pregnancy Association Evidence on Waterbirth (evidencebasedbirth.com) What Is Hydrotherapy And How Can It Help During Labor (mhealthfairview.org) Immersion in Water During Labor and Delivery | ACOG Skin-to-skin contact - Baby Friendly Initiative (unicef.org.uk) Here are some videos linked below that I’ve loved if you’re interested in what it could look like to have a water birth or use hydrotherapy for comfort: Home Birth Video using Hydrotherapy: (13 min) The Birth of Phoenix Jett Home Water Birth Video: (10 min) The Birth of Violet Water birth video in the Hospital: (24 min) The Birth of Meredith  Birth is a powerful, transformative process. Unfortunately, many people in the United States grow up believing that birth is simply something to be feared. It is hard work and emotionally & physically exhausting, but it doesn't need to be shadowed by fear but can be enveloped in peace when we mentally & physically prepare for it. It requires an openness to the journey & allowing your body to soften, open, release and surrender. Birth can be an empowering, sacred, beautiful experience. Birth is a natural part of a woman's life. The pain of contractions can be reshaped in our minds as power, pressure, intensity, energy, surges, rushes. Those strong sensations mean progress. One step closer to meeting your baby! All those years of cramping during periods have paid off! Your uterus has been preparing all your life for this moment of contracting and relaxing in a synchronized fashion to birth your baby. The muscle fibers of the uterus tighten and relax by the direction of a complex web of hormones that are purposed for labor.
These hormones are naturally occurring in our bodies and are most present when labor occurs without medications for augmentation or pain relief. If you are low risk, waiting for labor to occur when your body and baby are ready is the best chance of not needing to initiate, augment labor or use pain medications for the strong contractions brought on by artificial induction methods. The use of opioids or epidurals during labor can decrease these naturally occurring hormones from working effectively. Research shows that the effects of naturally occurring oxytocin and endorphins can be more powerful than morphine! For more info on oxytocin check out my blog post “Is Pitocin the same as Oxytocin?” I found it interesting to learn that women who have received pain medication in labor share more stories of how painful birth is compared to women who decided not to get an epidural or use other IV pain meds. In the hospital setting pain medications are readily available and it can be really difficult to turn down the offer of them during the intensity of a contraction or a long labor- even if you wanted to labor naturally. It can be helpful to include in your birth vision for your birth team that you'd like pain meds only by request and wouldn't like to have them offered routinely. Labor works best with privacy, a feeling of safety, and a total surrender to the process. Most mammals deliver in the darkness, where it is felt to be safe and intimate. Simulating this in modern birthing spaces can be done with thoughtfulness and care. Consider keeping the curtains pulled, having a sign that says “please knock” and if possible, choosing a birth location that allows for more privacy and a cozy atmosphere. Many cities have birthing centers or home birth midwives who are skilled at attending to low risk pregnant women. There is a lot of fear-based-advice & judgment surrounding many decisions about pregnancy, childbirth, postpartum and parenting. People tend to be quick to vent about their negative stories & hard moments and it can cloud the reality that every birth is unique. Every woman deserves to make her own informed choices and be free from judgement- no matter what she chooses! Practicing birth positions, relaxation techniques and learning about how your body was designed to birth your baby, during pregnancy can all help facilitate this release of tension & fear. There is no one size fits all approach to birth. You can choose to let go of other’s opinions and continue to trust your body, your carefully chosen birth team, your mama instincts, & the research you’ve put into making informed choices. Let’s stop the judgment projected over every choice & over sharing of negativity to new and expectant mamas and instead offer to help, ask if they are okay, if they need anything and support each other in peace, love & care and not fear. I believe in the power of story to transform and inspire. I hope you can enjoy positive, unique, birth stories and join in the community of women who are striving to let go of expectation, fear and welcome change, strength, relaxation & new life.
✨Hearing positive birth stories before and during pregnancy (through podcasts, books, friends & family) can be a helpful way to mentally & physically prepare for birth. ✨You have the power to prepare for your birth by inviting in peace and releasing tension & fear. ✨ You can choose to let go of other’s opinions and continue to trust your body, your carefully chosen birth team, your mama instincts, & the research you’ve done to make informed choices. ✨I highly recommend the book Ina May’s Guide to Childbirth. It completely opened my eyes to the possibility of birth filled with peace & not shadowed by fear. The @happyhomebirthpodcast is also my favorite podcast for learning about positive, natural birth stories. Women from all different backgrounds are invited to share their stories & learn from each other. It’s a beautiful, inspiring, & calming group of stories 💐  Creating a birth vision rather than a birth plan can empower you to envision what you'd like your birth & birthing space to be like knowing that birth is unpredictable. It can help you to learn about the risks and benefits of different interventions, make informed choices, and think through what you’d like to include in your birth, without focusing on controlling the birth but allowing the birth to unfold naturally. Patience for the journey & confidence in your body’s ability to birth are helpful to bring with you in labor! Let’s get started! You and your family deserve to have an empowered, beautiful, birth experience! If you’d like to learn more about the choices you have and would like help navigating the current research to make informed decisions, hiring a doula can be helpful! Envisioning your baby’s birth…
Some things to consider:
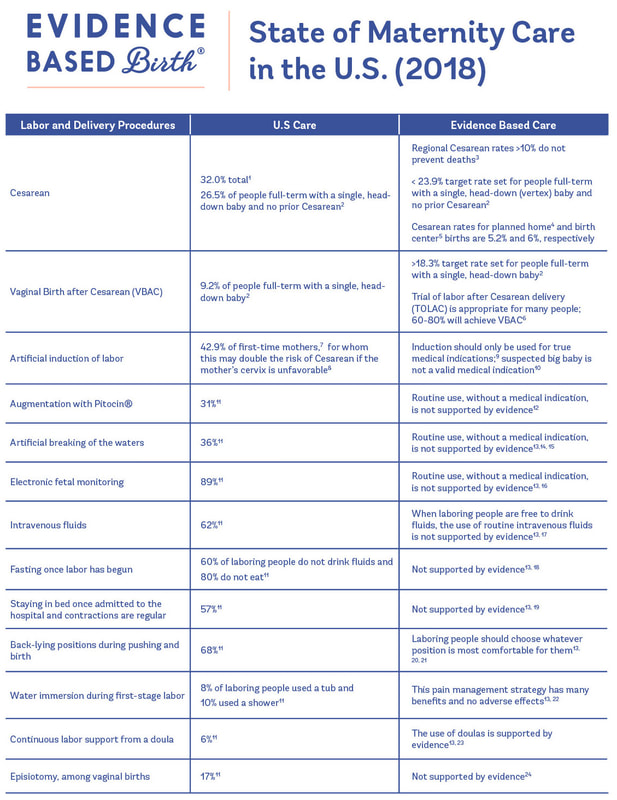
-Medical professionals skilled at attending low-risk births in the hospital, home or birthing center. Midwives can be found in many cities throughout the US, but in other developed countries Midwives are highly integrated into the health system caring for low-risk women during pregnancy, labor & postpartum, such as Germany, Canada, Denmark, Norway, and England, France and Australia to name a few. - Usually has a nursing background but not always. - Typically has a more holistic approach to childbirth and sees it as a normal part of a woman’s life and that it works best when left to unfold naturally. - Midwives are skilled at managing a variety of complications and transferring care to an OB if the mother becomes high risk. Obstetrician: - In most developed countries Midwives care for women in normal childbirth and work with OBs when the mother needs a physician to manage difficult births and complex situations because of their vast training in medicine! OBs also perform Cesarean births. - Due to the highly skilled training of labor and delivery, the focus is usually on the medical management of birth. Some interventions are not based on best practice for low-risk women and some of which can lead to what’s called ‘a cascade of interventions’ when not medically necessary (ex. Epidural or induction increases chances of using Pitocin which increases risk of fetal distress which can lead to requiring a Cesarean birth). Family Physician: Medical doctor who works primarily at a family practice and delivers babies in the hospital as well. . . Remember, this is your body, birth, & baby. You always have a choice for interventions, place of birth, midwife/OB, and you can always change your mind (Really, you can!) Creating a Birth Vision instead of a Birth Plan may allow you to be open minded to the unpredictability of birth. You can write this the way YOU WANT to. You can go into as much or little detail as you’d like. Sometimes, it is helpful to keep it less than one page double spaced and include only what you’d really like the doctors, nurses, midwives to know about you and your wishes. Medical providers, especially in the hospital, generally have multiple pregnant women in labor so the more concise the more likely they are to read it, remember it and respect your desires. Consider including a line that says something similar to: THANK YOU to my nurses and doctors/midwives for taking such good care of me! . . If you’d like to dive a little deeper...Check out the interesting, current research below! Midwives & Evidence Based Maternity Care: As you can see from this chart below, the only two developed countries listed that have more Ob-gyns than midwives are the US and Canada. (2) “In the U.S., certified midwives and nurse-midwives must hold a graduate degree from an institution accredited by the American College of Nurse-Midwives, and certified professional midwives must undergo at least two years of intensive training. This is designed to make midwives experts in normal physiological pregnancy and birth. Thus, for women with low-risk pregnancies who wish to deliver vaginally, it often makes sense to employ a midwife rather than a more costly surgeon. Yet only about 8 percent of U.S. births are attended by midwives.” (1) There are many medical interventions that are standard practice for birthing women. The research shows that what is commonly done in the US maternity care system is not based on best practice. See below for a chart from midwifery care Archives - Evidence Based Birth® that outlines some of these practices! References: Kegel Exercises By: Jan Mallak, 2LAS, AdvCD(DONA) What is a Kegel? Kegel exercises are basically pelvic floor toning or strengthening exercises. The pelvic floor has a figure 8 sling of muscles that surround the vagina and anus in women. These muscles support the bladder, rectum, and uterus. Why are they called Kegels? Dr Arnold Kegel (1894-1972) was an American gynecologist who noticed that childbirth weakened the pelvic floor muscles. So, he invented the perineometer to measure the strength of voluntary contractions of the pelvic floor muscles and he also recommended exercises as a non-surgical treatment of urinary incontinence from perineal muscle weakness or laxity. These exercises focus on the squeezing of the pelvic floor muscles by repeatedly contracting this hammock of muscles going from the front of the pelvis to the coccyx (tail bone). Why are Kegels beneficial? There are 7 reasons why Kegels are beneficial: 1. Improves overall fitness 2. Develops better back/hip support 3. Helps recovery after birth 4. Increases sexual satisfaction 5. Cures bladder leakage 6. Enhances pelvic health during menopause 7. Reduces chance of pelvic organ prolapse - This is when the bladder, rectum or uterus deviate from their initial bodily position. It can lead to leaking of urine or stool, a feeling of vaginal pressure/fullness and/or discomfort with sex. Prolapse is more likely when older and if there is a family history. So, you can see how doing Kegels helps before, during and after birth. It is a lifelong tool to use to maintain/improve health and reduce complications. Many maternity health care providers suggest doing Kegels to:
How are Kegels done? Some determine their pelvic floor muscles by stopping the flow while urinating for just a bit. It is not good to practice it this way, but it does help identify the muscle group and the effort made. The bladder may be incompletely emptied by stopping the pee midstream and that can lead to a Urinary Tract Infection. When can Kegels be done? When initially trying Kegels, sit comfortably in a chair with both feet on the floor and knees apart. Continue breathing normally while you purposely pull in and up on the muscles surrounding the vagina and rectum. As you become familiar and confident with these “contraction” techniques, they can be done anywhere and anytime. Like while standing in the grocery store line, driving, sitting at your work desk and even during sex! My favorites are while washing my hands after a bathroom break or during a red light. At 70, after doing these for decades, I can report that my pelvic floor health is very good (according to my doctor and husband of 50 years)! Which Kegel is best? There are Flicks, Super Kegels, and the Elevator Exercise. Flicks are what most people have probably heard about. Pull in and up on the muscles that you squeeze together when you are a block from home and really have to pee. Most women know what I am talking about! Generally, it involves a 10 second hold a few times done several times a day. Although it is better than nothing, it is like bending your arm at the elbow and touching your shoulder. Not too difficult and it really does not “tax” the biceps very much. The Super Kegel is the same idea but try to hold the muscles upward for a count of 20 seconds. If the muscles begin to fall, pull them back up. That would be like adding a 5 pound can of tomatoes to your hand and then touching it to your shoulder. It is harder work for your biceps, so more gain involved. Doing Super Kegels 6 times a day would be great. These are what I recommend for LIFE! The Elevator Exercise is also very beneficial – especially to prepare a woman for birth and in particular, for pushing. Sit in a chair and imagine that your bottom is the ground floor of an elevator at a department store. Now slowly lift the muscles a bit to the first floor and hold briefly, then a bit more to the second floor and hold briefly, and so on until the 5th floor (BABY DEPARTMENT!). Once you have reached the 5th floor, slowly lower the muscles to each decreasing floor until you reach the Ground Level. Now, BULGE you muscles downward to the BASEMENT floor for a bit - that simulates the act of pushing. You will feel your bottom pressing more against the chair – like when you are pressing the baby out. This can help coordinate your efforts when you may feel confused as to how to direct your downward power to birth the baby. Remember to keep breathing and loosen your jaw while doing any of these Kegels. Open moth = open vagina and relaxed jaw = relaxed pelvic floor muscles which means an easier birth. If you connect Kegels with something you do several times a day (like eating or using the bathroom), you are more likely to do it routinely. Some expectant moms put notes up around the house or at work as a reminder to do this important exercise. Kegels are sometimes called Sexercise because they can improve sensations during lovemaking - for both of you! In fact, dads can check the mom’s changing muscle strength if she squeezes his penis with Kegels during intercourse. What about men doing Kegels? Just like women, men have pelvic floor muscle but theirs encircle the base of the penis and support their bladder and bowels. If men copy stopping the flow of urine while tightening their buttocks, it is a Kegel. The penis will move a bit and the scrotum will lift somewhat. Kegels contribute to a man’s overall health, can enhance sexual performance, can reduce incontinence/dribbling and can help with bladder/erectile dysfunction. They may also alleviate some prostate problem symptoms, particularly after prostate surgery. A solid exercise plan for men is to do 3 sets of 10 short (3 seconds) and 10 long (10 seconds) Kegels twice a day. Thank you, Dr. Kegel! To summarize, Dr. Kegel gave both women and men an easy way to maintain their pelvic floor health and a therapeutic way to prevent or improve possible complications associated with the organs they support. So, thank you Dr. Kegel for your awareness, insight, knowledge, and expertise! Bio for Jan: Before recently retiring, Jan Mallak was a birth professional for over 40 years. During that time, she has functioned as a childbirth educator, birth/postpartum doula, doula trainer/mentor, doula service creator/coordinator, conference speaker, author, and birth consultant. Jan educated thousands of expectant couples, supported over a thousand doula clients, trained hundreds and hundreds of doulas, spoke at many local/national/international conferences, had countless articles/two books published and served in countless birth related volunteer capacities. Jan was one of DONA’s 17 initial Advanced Certified Doulas chosen worldwide and served as a Founding Board Member for the Mid-Atlantic Mothers’ Milk Bank in Pittsburgh. But she feels her greatest accomplishment and proudest moment was being her only grandchild’s doula almost 13 years ago (grandson Zeev). What to bring to the hospital/birth center:
Patience: The exact length of labor is unknown. For first time mothers labor is typically longer than women who have birthed before, but that too can vary. My tip would be to assume it will take a long time. Let the medical team focus on the clock and, as much as you can, dive into laborland with your partner. This will relieve you of unnecessary stress and let you be more present. Learning the stages of labor is helpful but know that most people forget this during the heat of the moment - that is okay! You aren’t supposed to be a medical professional- just lean into each moment and help her through each breath and each contraction. That being said, most midwives and doctors follow a standard for you to follow for when to go to the birthplace. Most use the 5:1:1 rule (contractions 5 minutes apart for 1 minute for 1 hour) but follow the instructions of your provider and then let them do the rest of the time keeping when you arrive! “When you allow yourself to be immersed in labor, it is neither boring nor interesting, because the very nature of labor dissolves ordinary boundaries of time and space. You and labor become one. Timing your labor requires remaining conscious-of-self rather than being-in-labor” (England & Horowitz 1998). Presence: Having a doula allows you to step out of the room to make a quick call to update family if desired, use the bathroom, eat a sandwich etc... doing these things in front of your wife/partner during certain times in labor may make her lose concentration and increase pain. Pro tip: Turn off your phone Positive Words: Your wife/partner will feed off your energy. If you are calm, confident, strong, reassuring and patient, she will naturally be more relaxed, and labor will progress more smoothly and less painfully. The more you relax and lean into labor, the more she will be able to let go of control and release tension. It is hard to see the one you love in pain but know that the pain is purposeful. Try different positions, comfort measures, encouraging words, calm and strong back, hand, inner thigh, foot massages, singing to the baby, and match her breathing. If you notice she is making noises don’t discourage but allow her to express her emotions and sensations how they come naturally. Vocalizing in labor: In our culture, it is often frowned upon to be vocal in labor but often these noises are helpful in releasing tension, allowing the baby to move down, and to cope with the pain. Deep, guttural, low moaning/grunting/yelling are the most effective and should be encouraged. If you start to notice her voice rising in pitch or sounding more like screaming, she may be producing these from a place of fear, and this can make her tire out and have less effective contractions. On the next contraction, encourage her to make her voice deeper, you can try matching her sounds as well. Some women are introspective and quiet, some are loud, vocal, yelling, talking, all are natural and there is no ‘right’ way to act/be! Labor Project: Early in labor, it may be helpful to plan a fun activity together; strolling through Target (who doesn’t love Target, let’s be honest), washing & folding baby clothes, baking a birthday cake, gardening, maternity photo shoot, going for a walk through town etc. This can be a good distraction before labor really picks up and will help keep things moving and progressing using gravity. [There is a great chapter on this in the book Birthing from Within.] Join in: If she is walking, rocking, swaying, dancing- join in! Doing so may make her feel less alone and more supported. If she is drinking water, drink some water. Staying hydrated yourself will preserve your energy too. It’s easy to forget about yourself when you are focused on her! Drinking fluids will also remind her to keep hydrated; win-win! Watch & Wonder Her body was created to grow and birth your child. It has been shown that for women who are low risk, labor works best when allowed the freedom to unfold naturally. As the father/support person, your role is to watch, wonder, marvel at the rollercoaster of labor and birth, and support her in comforting ways. Having a doula and a medical provider (midwife or OB) who you trust allows you to relax a little, knowing you are on the same team. Choosing a Care Provider: Medical intervention during birth is very important in certain circumstances and we are lucky to have access to hospitals who can provide treatment when necessary. Unfortunately, many hospitals have policies that are standard practice for everyone, not just women who are at higher risk. Know that you always have a choice for interventions and educating yourself prior to labor will help you to make informed decisions. It is important to find a care provider who listens well and makes you feel comfortable asking questions. It is (almost) never too late to change to a different OB or choose a midwife! Midwives are skilled birth attendants who care for low-risk pregnant women who tend to allow birth to unfold naturally and only intervene when medically necessary, whereas many Obstetricians (OBs) are trained to be obstetric surgeons who perform Cesarean births. They also deliver most babies in the United States and because of their highly skilled training, tend to take a more medical approach to birth. In many other developed countries, midwives are more common than OBs for low-risk pregnant women. Depending on your preference in care, in some hospitals, you can choose to have an OB or Midwife as your provider. In many cities, there is a birthing center where midwives attend low risk births. If you are unsure why an intervention is being introduced, ask your provider for all the information you & your partner need to make an informed decision. Your doula is also there to support you in making an informed choice and help you to advocate for yourself- but does not make decisions for you or speak for you. General tips:
References: England, P., & Horowitz, R. (1998). Birthing from within: An extra-ordinary guide to childbirth preparation. Albuquerque, N. M: Partera Press.  You may have heard that Pitocin and Oxytocin are essentially the same, but there are crucial differences that are helpful to know when making decisions before, during and after birth. What is Oxytocin? Oxytocin is a naturally occurring hormone produced in the hypothalamus and released by the pituitary gland into the bloodstream and circulates throughout your entire body including your brain. What is Pitocin? Pitocin is a synthetic version of oxytocin that is chemically identical although they have significant differences. Pitocin is injected into your bloodstream through an IV (usually) and is not able to cross what's called the blood brain barrier, therefore it does not have an effect on the brain. (3) What does Oxytocin do to help labor? Oxytocin is sometimes referred to as the love or cuddle hormone. It is produced when we feel safe, warm, and loved. Sex, kissing, hugs, lactation, and labor contractions all cause increased oxytocin production. Oxytocin is produced by your body to increase intensity and frequency of labor contractions to bring your baby earth-side but because it crosses the blood brain barrier, it also signals to the brain to produce beta-endorphins- which have been shown to be 18-33 times more potent than morphine! (1) This calming, pain reducing, protective mechanism, that our body creates for us during labor, is helpful for moving through the pressure and strong sensations of labor. Oxytocin peaks towards the end of labor, giving the mother a rush of the morphine-like effects to decrease pain sensations in the pushing stage of labor as well as immediately after birth. This peaking of oxytocin also creates what's known as the fetal ejection reflex in some women, where the baby is birthed more quickly and easily, without the mother working hard to push the baby out. Oxytocin also improves mother/baby bonding and improves breastfeeding in the initial time after birth known as the “Golden Hour.” Why is Pitocin used during birth? Often Pitocin is offered for induction of labor (starting), augmentation of labor (speeding up), and to prevent or treat postpartum hemorrhage. Because Pitocin is given as a slow, continuous IV medication during labor, it has been shown to make labor pains more intense without the protective, pain reducing effects that naturally occurring oxytocin provides. This increase in pain sometimes leads women to choose an epidural which can decrease ability to move around during labor, cause labor to slow down, and decrease ability to push on your own because of decreased sensations. The slowing down of labor with epidural use can increase the need for a higher rate of Pitocin which leads to even stronger contractions. These stronger contractions brought on by Pitocin can increase the risk of fetal distress and may result in the necessity of a cesarean birth. “Mothers who have labored with and without Pitocin usually report that contractions augmented by Pitocin are much more painful, which may be due to increased intensity of contractions and low levels of beta-endorphins.” (2) Why is Pitocin used after birth? Some hospital policies having standing orders- meaning automatically done for every mother, to infuse Pitocin immediately after birth to prevent postpartum hemorrhage by increasing uterine contractility. The nurses also massage the fundus- the name for the uterus, which helps to stimulate the uterus to contract and shrink into a ball, so you don’t bleed too much after birth. To learn more about the current evidence of using Pitocin to prevent postpartum hemorrhage I encourage you to read the article from Evidence based birth linked here: Evidence on: Pitocin® During the Third Stage of Labor - Evidence Based Birth® To summarize, Oxytocin and Pitocin are both chemically identical hormones that facilitate the progression of labor by bringing on contractions and causing the uterus to contract after birth to prevent hemorrhage. However, they are different in important ways because the synthetic form called Pitocin does not have the morphine-like effects of Oxytocin that decrease pain and thereby decrease the risk of requiring other interventions during labor. Cuddle, kiss, dance, hug, ask for a back massage- these intimate things may help your body release protective endorphins that can decrease pain and promote baby's progress through your body and into your loving arms! For some women, using Pitocin to induce or augment labor is a medically indicated choice (ie. induction related to high BP, preeclampsia, postdates etc). However, many women are encouraged to use Pitocin during labor to “speed things up,” when it can lead to increased pain and medical interventions. Women should be educated on the risks and benefits of using Pitocin during labor and the incredible benefits for both mom and baby of allowing natural oxytocin to flow when possible. References/resources if you’d like to learn more!
 For thousands of years, women across the globe have been giving birth in countless positions. Most images and stories of women during labor, historically, have been in upright positions; walking, squatting, bouncing, dancing, leaning etc. When the majority of births in the West shifted to the hospital in the early twentieth century and the use of general anesthesia became commonplace, women were often strapped to the bed and told to lie flat, in large part because it was easiest for the doctor to see. Although general anesthesia is rarely used today, unless in the necessity of an emergency Cesarean birth, the most common birthing position continues to be lying back positions. Some of this can be attributed to many women choosing to have an epidural during labor which often restricts movement (although there are positional changes you can make with an epidural- with assistance!) Current research supports movement in labor and birth and I encourage you to dig deeper into the history if you’re interested! It is important that you are comfortable asking question to your chosen provider (OB, Midwife, Family Physician). It is ideal to have a provider who understands the benefits of frequent positional changes. Let's get into it! There is no "right" way to birth. Listen to your body, your care provider, and your doula. If something feels off or you've been in the same position for a while- try changing it up. You may surprise yourself which position you like best so try a few different ones! Utilizing gravity and being active in labor optimize the baby's descent into and through the birth canal. Upright Labor & Birth Positions (some examples):
Evidence Based Suggestions:
Resources/References: Articles:
“The Birth Partner”- Penny Simkin (2013) “Doula’s Guide to Birthing Your Way”- Jan S. Mallak (2010) “Ina May’s Guide to Childbirth”- Ina May Gaskin (2019) "Birthing From Within" - Pam England & Rob Horowitz (1998) “Hygge has been called everything from “the art of creating intimacy,” “coziness of the soul,” and “the absence of annoyance,” to “taking pleasure from the presence of soothing things,” “cozy togetherness,” and my personal favorite, “cocoa by candlelight”.” ― Meik Wiking, The Little Book of Hygge: The Danish Way to Live Well Hygge [pronounced hyoo·guh] is a Danish & Norwegian word and has been culturally embedded into the Scandinavian people. It has recently been taken up by people all over the world who are searching for ways to embrace the coziness and simple joys of life. It can also be used as an adjective to describe something that has 'hyggelig' qualities.
Hygge is about connection; with nature, ourselves, family & friends. It is the feeling of warmth and contentment you get from a candlelit atmosphere and fuzzy socks. When you experience Hygge you feel cozy and safe. From Meik Wiking in his book The Little Book of Hygge, he includes elements of hygge to be candles, having friends over to share a meal, slowing down and allowing yourself to be present and live in simple, cozy spaces. It includes a generous amount of movement and getting outdoors for fresh air and nature walks. It is a delightful little book filled with ideas of ways to be more grateful for the little joys in our day to day lives. It surprised me how much a book would make me want to go out and buy a sheepskin for my couch- for the hyggelig effect! • • • “Hygge is humble and slow. It is choosing rustic over new, simple over posh and ambience over excitement. In many ways, hygge might be the Danish cousin to slow and simple living.” ― Meik Wiking, The Little Book of Hygge: Danish Secrets to Happy Living Now.. onto the main topic of how embracing Hygge can be applied to the realm of birth and postpartum care! HYGGELIG BIRTH The idea of shaping your birth space and vision with people and things that bring a feeling of hygge to you is helpful not only to 'feel cozy' but it actually physiologically helps you in the birthing process. Birth is powerful & so are you. It is challenging and hard and deserves awe for the process. When we feel feelings of fear, scarcity or anxiety our body produces fight or flight hormones that cover the ‘cuddle hormone’ oxytocin that helps labor to progress naturally and effectively. When we feel safe, comfortable, known, cared for and loved, oxytocin stimulates the release of dopamine and serotonin (other 'feel good' hormones in the brain) to increase relaxation and confidence & decrease our sense of pain. Isn't that incredible?! Your Doula should be someone who you feel safe and comfortable with and a person who you trust to be with you in your birthing space; enhancing your partners ability to care for you. Your husband/partner plays an important role in giving you boosts of oxytocin with his/her calm presence and comforting massages. Don't be afraid to kiss & snuggle- it just might allow you to relax and progress more quickly in your labor! In all birth environments [whether you choose: your home, hospital or birthing center] there is a type of planning that is required to ensure you feel safe and comfortable during labor. For example: choices surrounding privacy during labor, types of interventions/monitoring devices, dim lights/bright lights, which comfort items you bring with you, clothing you choose to wear, people you invite to the birth and to visit afterwards etc. Start thinking now of comfort items, support people, environmental considerations you'd like to make to have a Hyggelig birth space to welcome your baby into! POSTPARTUM The postpartum period is often defined as the first six to eight weeks after your baby is born. This is split into two phases; the first ten days after the baby arrives and then up until eight weeks. In the United States there is often a lack of support for women and their families to have education for what to expect in this period as well as appropriate follow up. Women who are unsupported during this time have higher rates of postpartum depression, infant feeding issues, and can even have long term lack of confidence in their role as a mother. This is where the role of the postpartum doula comes in! Postpartum doula support varies for each person depending on their need. This type of doula work involves light cooking/cleaning, swaddling baby, newborn care teaching, help with nursing/referral to a lactation consultant if indicated, an opportunity to process the birth, as well as tips for postpartum healing and infant soothing techniques. This is a specific type of doula but most birth doulas (including myself) provide support in the postpartum period during follow up visits and in the form of additional hours (included in certain birthing packages). HYGGE IN POSTPARTUM You should be hiding granola bars in your couch cushions. [When you find yourself sitting on your couch with a newborn nuzzled onto your chest, enjoying cozy closeness with your little one and then you realize you haven't eaten anything and you'll be there for 20-40 minutes.. you might be glad you have those granola bars! haha] In all seriousness, planning the postpartum period is IMPORTANT and should be done carefully and thoughtfully. The Hygge concepts I think of when planning for after baby arrives are: planning your nursing space (large water bottle, comfy & supportive chair, snacks, blankets etc), inviting friends and family to help with meals for several weeks (https://www.mealtrain.com/), and planning your healing and transition in this time that is often called the "fourth trimester." I generally recommend the 5-5-5 "rule" for postpartum. More on this and tips for postpartum to come in another post. Planning the first weeks postpartum can be daunting; hiring a doula can help you prepare for this time so you have the confidence and reassurance you have a good, supportive plan in place! References: Team, A. B. (2020, August 28). Serotonin and the other happy hormones in your body. Atlas Biomed blog | Take control of your health with no-nonsense news on lifestyle, gut microbes and genetics. Retrieved November 24, 2021, from https://atlasbiomed.com/blog/serotonin-and-other-happy-molecules-made-by-gut-bacteria/#:~:text=These%20hormones%20or%20neurotransmitters%20are,oxytocin%20is%20the%20cuddle%20hormone. Books for Continued Learning:
|
Archives
May 2023
Tip:To see the blog posts from each month, click the links above under Archives. |